Get to Know Vaya
Embracing whole-person care by nurturing the mind, body, and spirit
Who We Are
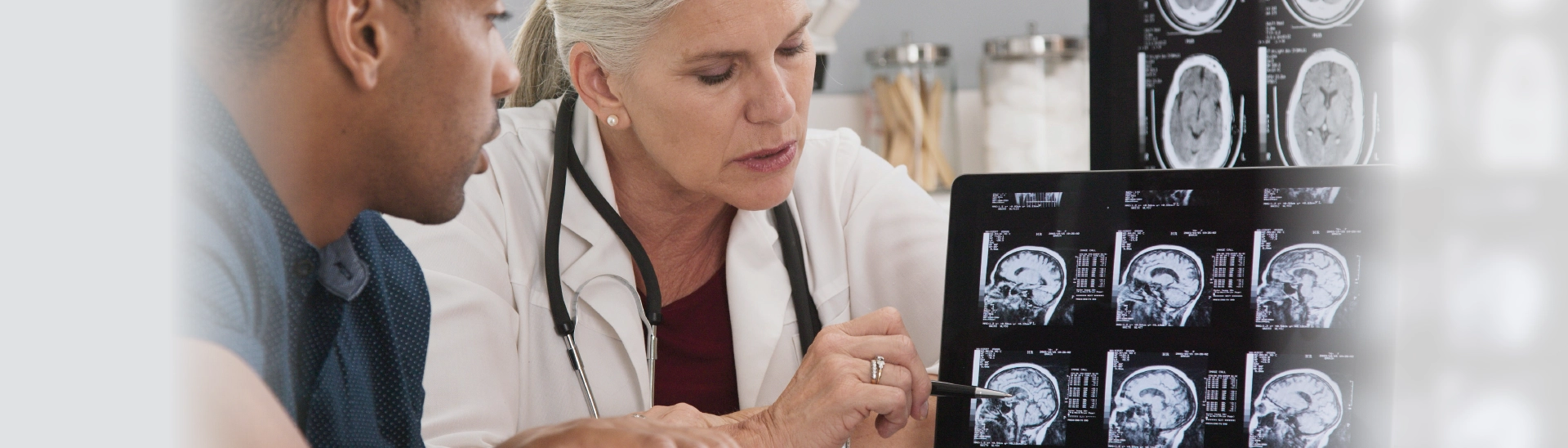
Vaya Health is a public managed care organization (MCO) that prioritizes whole-person health. We manage Medicaid, federal, state, and local funding to connect the people we serve to health care services and supports. Our specialty is helping individuals with needs related to mental health, substance use disorders, intellectual/developmental disabilities (I/DD), and traumatic brain injuries (TBI). We strive for members and recipients to receive the right care, in the right amount, at the right time.
Serving North Carolina
To manage prevention, treatment, and crisis services, we partner with more than 4,000 health care organizations and practitioners across North Carolina. This network provides person-centered care to help people on their path to health and wellness. We manage two health plans:
Behavioral Health and Intellectual/Developmental Disabilities Tailored Plan
- We manage mental health, substance use, I/DD, TBI, physical health, and pharmacy services, as well as Long-Term Services and Supports, for Medicaid beneficiaries. These individuals are referred to as Vaya Total Care members.
- We manage mental health, substance use, I/DD, and TBI services for individuals without insurance – or too little insurance – who are eligible for care funded by the state of North Carolina or other public funds. These individuals are referred to as Tailored Plan recipients.
NC Medicaid Direct Prepaid Inpatient Health Plan
- NC Medicaid Direct is North Carolina’s health care program for Medicaid beneficiaries who are not enrolled in managed care plans. Vaya is responsible for managing mental health, substance use, I/DD, and TBI services for these individuals, who are referred to as NC Medicaid Direct members.
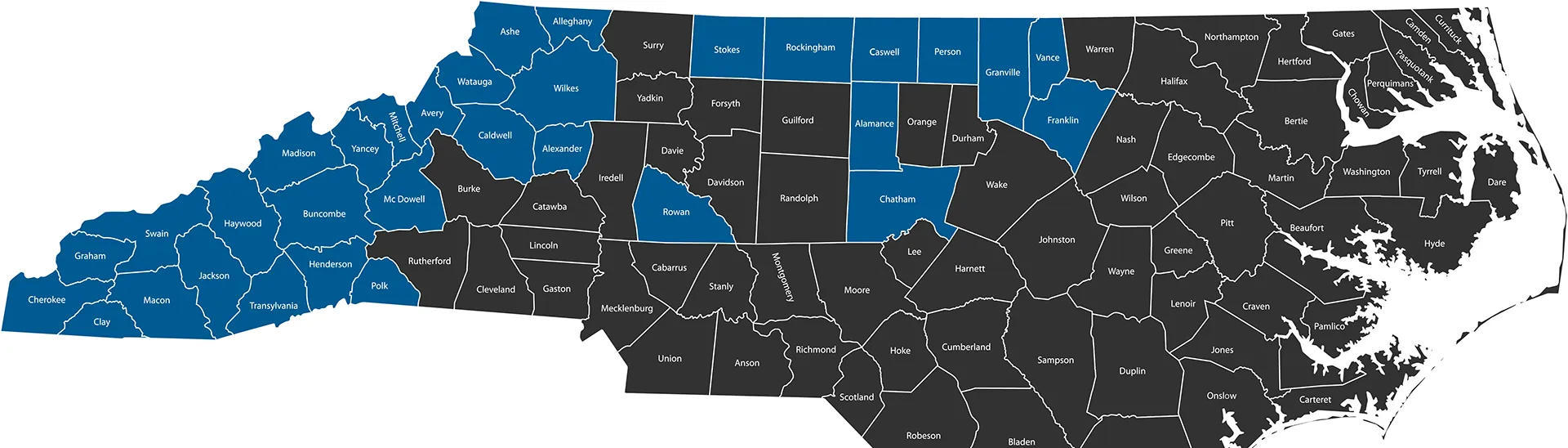
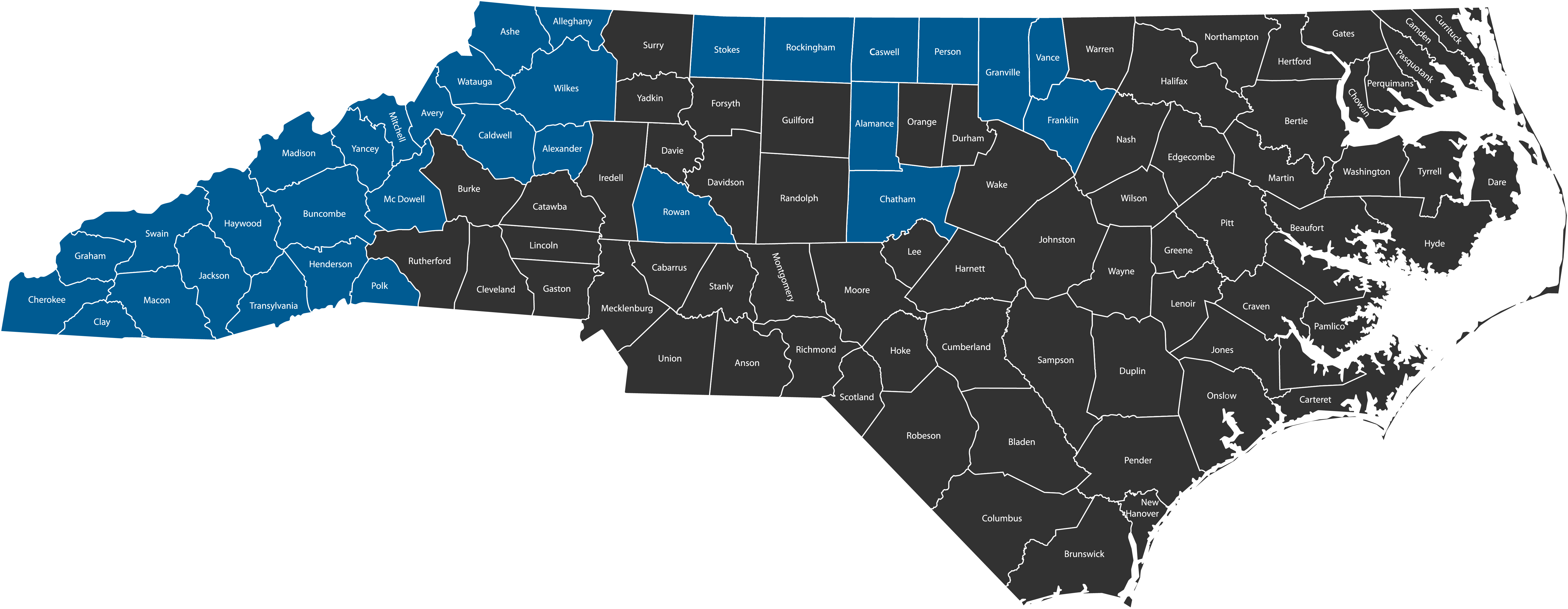
Vaya Counties
We currently offer both health plans in the following North Carolina counties: Alamance, Alexander, Alleghany, Ashe, Avery, Buncombe, Caldwell, Caswell, Chatham, Cherokee, Clay, Franklin, Graham, Granville, Haywood, Henderson, Jackson, Macon, Madison, McDowell, Mitchell, Person, Polk, Rockingham, Rowan, Stokes, Swain, Transylvania, Vance, Watauga, Wilkes, and Yancey.
Our Mission, Vision, and Values
MISSION: “Who We Are”
Members are our mission. Technically, this means we manage publicly funded care for individuals with a mental health condition, substance use disorder, I/DD, and/or TBI. We exist to benefit the lives of people with mental health, substance use disorder, I/DD, and TBI needs and manage the medical, behavioral, and non-medical drivers of their health. What this means is that we organize care to connect people with the services and supports they need to live their best lives. We strive for members to receive the right care, in the right amount, at the right time.
VISION: “What We’re Building”
Communities where people get the help they need to live the life they choose. We are committed to meeting local needs through collaboration with county partners, on-the-ground decision-making, creative problem-solving, and consistent follow-through. We focus on listening to each area’s unique needs and developing solutions that will support the best outcomes for the individuals and communities we serve. Our goal is to successfully evolve in the health care system by embracing innovation, adapting to a changing environment, and maximizing resources for the long term benefit of the people and communities we serve.
VALUES: “What We Believe In”
We believe in the power of recovery, that peer support is a critical part of the care continuum, and that integrated, person-centered care is the best approach for treating each individual as a whole, unique person.
- We care about the individuals we serve and the people and organizations who serve them.
- We are passionate about improving public health in the communities we serve.
- We believe that health care should not be about profit.
- We operate with integrity, which means ensuring quality care and accountable financial stewardship through ethical, responsive, transparent and consistent leadership and business operations.
We believe that person-centeredness means interacting with compassion, cultural sensitivity, honesty and empathy; that integration means caring for the whole person within the home and community of an individual’s choice; and that we demonstrate commitment by partnering with members, families, providers, and others to foster genuine, trusting, respectful relationships essential to creating the synergy and connections that make lives better.
Our History
Vaya’s roots in North Carolina go back to 1972. Today, we serve residents of 32 counties across the state. Alongside our members, recipients, providers, and community stakeholders, we are moving forward together toward a healthier North Carolina.
As an area authority in 1972, we provided direct services and operated facilities in the state’s seven westernmost counties.
In 2001, North Carolina implemented reforms related to public behavioral health and I/DD service delivery. We transitioned from an area program to a local management entity (LME), ceasing direct service provision and managing care delivered by area providers. We went on to successfully complete mergers with neighboring LMEs to our north and east.
In June 2011, the state Legislature expanded the Medicaid 1915(b)/(c) Waiver statewide, moving all mental health, substance use, and I/DD services into a managed care delivery system. We transitioned to a full LME/MCO on July 1, 2012, serving both Medicaid members and State-funded services recipients. In 2013, we merged with another LME/MCO, Western Highlands Network.


To better reflect our commitment to moving forward and improving public health and well-being, in 2016 we changed our name to Vaya Health. We care about the people we serve, those who provide their care, and the communities they call home.
The Boards of Vaya and Cardinal Innovations Healthcare announced their decision to consolidate in June 2021, expanding Vaya’s geographic footprint to 32 counties across the state. One month later, in July 2021, Vaya was awarded a contract to operate a regional Behavioral Health and I/DD Tailored Plan as part of the state’s transition to NC Medicaid Managed Care. In 2024, our region expanded to add Rockingham County.
Our Team
At Vaya, whole person care isn’t just a pursuit—it’s our passion. We’re inspired by the people and communities we serve. Our staff understand the journey to well-being may not always be a straight line, but we’re here for members and recipients every step of the way.
Looking for a place to put your passion to work? Let’s move forward together.


Leadership and Governance
As managers of public funds, we strive to ensure access to quality care for those we serve and accountable financial stewardship in our daily operations. Vaya’s leadership works closely with our governing Board of Directors and four Regional Boards to align efforts to best meet the needs of our communities.
Advocacy and Involvement
Our vision is to build communities where people get the help they need to live the life they choose. We’ve seen Vaya members, recipients, and local communities give back and get involved in their care, education, and overall health. We welcome stakeholder participation in what we do. That includes opportunities to serve on key committees and participate in quality trainings and education.